EYE DISEASES
Each part of the eye plays an important role in protecting your vision and providing you with a clear and healthy one. However, certain factors such as extreme exposure to UV, aging, hereditary, and unhealthy lifestyle can lead to certain eye diseases.
Below are just some of the few eye diseases that are common in the Philippines.
What is CATARACT?
Imagine yourself seeing a foggy, hazy glass and everything seems to be a blur. But in reality it’s a crystal clear glass and you are the only one who is seeing it differently. If this is the case, you might be having a CATARACT, a clouding of the lens that can either be caused by age, family history, diabetes, intake of steroid, or an eye injury to name a few.
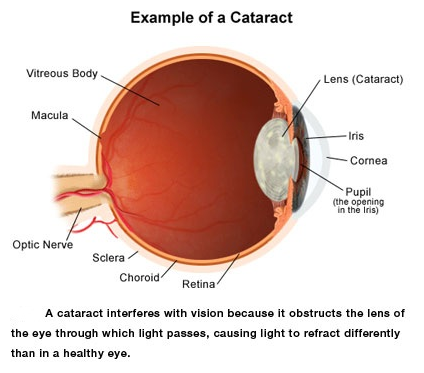
CATARACT is the most common cause of blindness worldwide. In the Philippines, 62% of all blindness is caused by it and found mostly in older age groups. (http://www.doh.gov.ph/national-prevention-of-blindness-program)
CAUSES OF CATARACT:
Like a camera, the eyes have lens that lies behind the iris and the pupil. It focuses light or an image on the retina and adjusts the eyes focus to make us see things clearly whether near or far. The lens is made up of protein and water. However as we age, the proteins clump together causing the lens to be clouded which now forms a cataract. Over time, the clouds may grow in size which makes light difficult to pass through it.
It is best advised to consult with an Ophthalmologist to prevent blindness as this can be treated at an early stage through surgery and implant of Intraocular Lens (IOL) to regain back a normal, clear vision.
BEST TO CONSULT WITH: General Ophthalmologist
What is GLAUCOMA?
Like a modern DSLR camera, we usually take pictures from it, connect it to a computer using a cable and download the image.
The eye is like the digital camera where an image is initially stored, while the cable wire is the optic nerve that sends signals to the brain, which is the computer. If the cable wire (the optic nerve) is damaged, it won’t be able to transfer or send files to the computer (the brain) in order for us to see. But unlike the damaged cable wire, the optic nerve cannot be repaired.
GLAUCOMA is the name given to a group of related diseases where the optic nerve is being damaged resulting to irreversible blindness. The nerve fibres progressively die taking away the peripheral or side vision first. Usually called the “Silent Thief of Sight”, visual loss goes undetected until it is quite advanced. It is also the second leading cause of blindness worldwide.
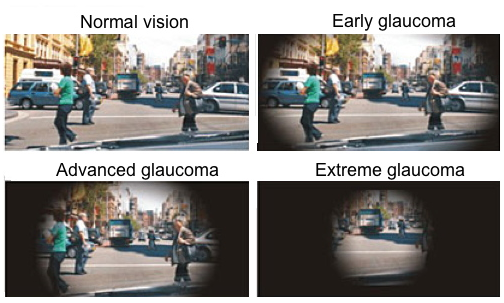
Photo Source: National Eye Institute
A person who has a family history of glaucoma and diabetes, is over 40 yrs old, and have high intraocular pressure may have a higher risk or chances of having one. Most often, Glaucoma patients will not experience any symptoms.
It is best to have a regular eye check for early detection and to prevent glaucoma from getting worse. Remember, reading 20/20 does not mean your eyes are healthy. Make sure the doctor checks your eye pressure with tonometry every 2-3 years, or more often if you family history.
BEST TO CONSULT WITH: Glaucoma Specialist (link to list of Perfect Sight Eye Center’s Glaucoma Specialist)
What is MACULAR DEGENERATION?
Unlike Glaucoma where peripheral vision is affected, MACULAR DEGENERATION (MD) OR AGE RELATED MACULAR DEGENERATION (AMD) affects the central vision of the eye. The macula is the 3-5mm area in the retina that is responsible for the central vision. Blurring of words on a page, difficulty recognizing features on a face, dark areas in the center of vision, and/or distortion of straight lines are some of the effects of this type of eye disease.
As the names suggests, it usually occurs as part of the ageing process. Aside from its natural cause, hypertension, smoking and exposure to UV rays are just some of the possible factors of AMD.
There are two types of AMD - Dry AMD and Wet AMD.
The Dry AMD, which is the most common form, is caused by aging and thinning of macular tissues.
WET AMD is caused when abnormal blood vessels forming underneath the retina. These vessels leak blood and or fluid and blur the central vision. Vision loss may be rapid and severe.
There are treatments that can help like anti-VEGF (vascular endothelial growth factor) injections. It is an antibody which inhibits leakage and growth of new vessels. There are three variansts eg Lucentis, Eylea, or Avastin. Our Retina doctors will help you decide on which is best for your eye.
BEST TO CONSULT WITH: Retina Specialist

What is DIABETIC EYE DISEASE?
Do you have a poor control of sugar intake?
You might want to slow it down as you age. Aside from hearing loss and foot complications to name a few, Diabetes can also lead to blindness. Not only can it lead to Cataract, it can also lead to two (2) conditions:
Early on, diabetic retinopathy is asymptomatic, so once you are diagnosed with diabetes, please have your eyes checked by your Ophthalmologist.
1. DIABETIC RETINOPATHY, a condition which involves changes to retinal blood vessels that can cause them to bleed or leak fluid, distorting vision. It is the most common cause of vision loss among people with diabetes and;
2. DIABETIC MACULAR EDEMA, a result of diabetic retinopathy which involves swelling and accumulation of fluid (edema) in the macula.

DIABETIC RETINOPATHY has four stages – 1. Mild 2. Moderate 3. Severe and 4. Proliferative. As the stages progress, more blood vessels that nourish the retina are blocked until it triggers growth of new blood vessels that have thin, fragile walls that can leak blood which results to severe vision loss and even blindness.
DIABETIC MACULAR EDEMA (DME)
The macula is responsible for the sharp, straight-ahead vision that is used for reading, recognizing faces, and driving. Too much fluid in it can affect vision permanently. Those who have Diabetic Retinopathy are most likely to develop diabetic macular edema (DME).

Photo from: http://www.scienceofdme.org/learn/
Those who have diabetes (type 1 and type 2) are highly suggested to take an annual comprehensive dilated eye exam. These includes:
Visual Acuity Testing – measures ability to see at various distance
Tonometry – measures pressure inside the eye
Pupil Dilation – widens the pupil to examine retina and optic nerve
Optical Coherence Tomography (OCT) – like an “ultrasound” that uses light waves to see detailed images of tissues such as the eye
Depending on your initial tests, your Ophthalmologist may require other tests not mentioned above.
It is best to have an eye exam as early as possible if you are diagnosed with diabetes. It can reduce risk of blindness up to 95% with timely treatment and proper control of sugar and blood pressure.
BEST TO CONSULT WITH: Retina Specialist (link to list of Perfect Sight Eye Center’s Retina Specialist)
EXTERNAL DISEASE AND CORNEA
The cornea is the outermost portion of the eyeball which plays a crucial role in focusing the vision. It is situated in front of the iris (colored part of the eye) and meets the sclera (white part of the eye) at an area called the limbus. The cornea is inherently devoid of blood vessels and it is nourished by the tears, the aqueous humor (fluid that fills the space behind it), and the surrounding conjunctival blood vessels. As it is the most exposed part, it is prone to a lot of environmental hazards such as UV radiation, foreign body, irritants, allergens, and trauma from contact lens use, chemicals, mechanical causes, etc.
Below are some of the common diseases affecting the cornea and external eye in the Philippines:
What is PTERYGIUM?
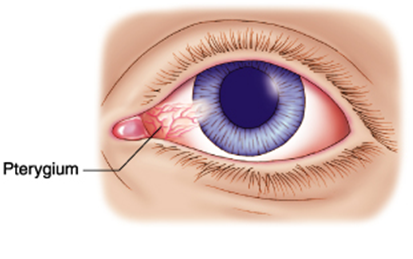
Pterygium, which is locally known as “pugita,” is a pinkish, triangular tissue growth commonly seen on the exposed part of the cornea, starting from the limbus and eventually grows toward the center of the cornea. It is caused by too much exposure to UV radiation from the sun, therefore it is usually seen in countries with a tropical climate like the Philippines. Those who work under the heat of the sun like farmers, fishermen, and seamen, and those who are actively outdoors are more prone to having one.
SYMPTOMS
The most common symptom is the note of a fleshy mass on the nasal limbus. Other symptoms are redness, pain, foreign body sensation, tearing, and blurring of vision in advanced cases.
TREATMENT
Early in the disease, treatment may be confined to lubrication for symptom relief. Surgery is reserved for advanced cases because simple excision of the mass is prone to recurrence, especially in patients under 40 years old. Combining the excision with other surgical techniques such as conjunctival autograft or amnion graft decreases the risk of recurrence after the procedure.
What is DRY EYE SYNDROME?
Are you experiencing a sandy or gritty feeling in your eye? How about stinging, burning feeling? You might be experiencing DRY EYE SYNDROME.
Dry Eye Syndrome occurs when there is either rapid evaporation or insufficient production of tears. Tears are necessary for over-all eye health and clear vision.
SYMPTOMS
Patients with dry eye syndrome often experience redness, tearing, eye discharge, eye pain, foreign body sensation, itchiness, blurring of vision, photophobia, glare, and eye fatigue. These symptoms are usually observed towards the afternoon or night time or during reading, watching, using the computer and other gadgets. It can also be exacerbated by hormonal changes, contact lens use, very hot or very cold weather, allergies, and some oral and topical medicines.
POSSIBLE CAUSES:
Dry eye syndrome may be classified into 2: AQUEOUS TEAR DEFICIENT and EVAPORATIVE. Aqueous Tear Deficient Dry Eye Syndrome is due to insufficient tear production and may be caused by aging, menopause, contact lens use, diabetes, cataract and refractive surgery and side effects of certain medicines. Evaporative Dry Eye Syndrome is due to fast tear evaporation and may be caused by blepharitis, allergic conjunctivitis, prolonged reading, watching, use of computer and other gadgets, contact lens use, Vitamin A deficiency, and side effects of certain medicines.
TREATMENT
Lubricants are the mainstay of treatment for Dry Eye Syndrome. Anti-inflammatory medications eg Cyclosporine drops may be given. Omega-3 fatty acid supplement may also be given as adjunct to treatment.
What is SORE EYES or CONJUNCTIVITIS?
Conjunctivitis or sore eyes is the inflammation of the conjunctiva, which is a membrane covering the sclera and the inner part of the eyelids. The most common type is caused by adenoviral infection. Usually lasting from 5 – 12 days, it occurs usually during summer or rainy season of which viral respiratory infections such as influenza or adenovirus is higher.
SYMPTOMS
Patients usually complain of eye redness, swelling, tearing, discharge, stinging, itching, and discomfort.
TREATMENT
Most conjunctivitis is viral and may resolve without treatment. however, decongestant drops are usually given to relieve the discomfor. Bacterial conjunctivitis may be given antibiotic drops to shorten the course and avoid the spread of the disease. It is important to note that it is unsafe to self-medicate because some eye drops are contraindicated in certain eye diseases with similar presentation. Frequent handwashing and hygiene is also a vital component of the management.
TIPS TO AVOID SORE EYES
● Wash your hands frequently and thoroughly with soap and water.
● Do not borrow another person's eyewear, makeup, handkerchief or towel.
● Wash clothes, towels, pillow cases, and anything else which may have come in contact with an infected person.
● Minimize hand-to-eye contact.
● On windy days, wear eyeglasses or sunglasses to protect your eyes from foreign particles
● Disinfect surfaces such as doorknobs, computer keyboards, counters and handrails with a diluted bleach solution.
WHAT TO DO WHEN YOU SUSPECT SORE EYES
Artificial tears and cold compress may be started to alleviate the symptoms. However, consultation with an ophthalmologist is still highly advised.
